What are CAR-T Cells?
CAR-T cells represent a major breakthrough in cellular immunotherapy for cancer. These genetically engineered T lymphocytes are designed to specifically recognize and destroy cancer cells.
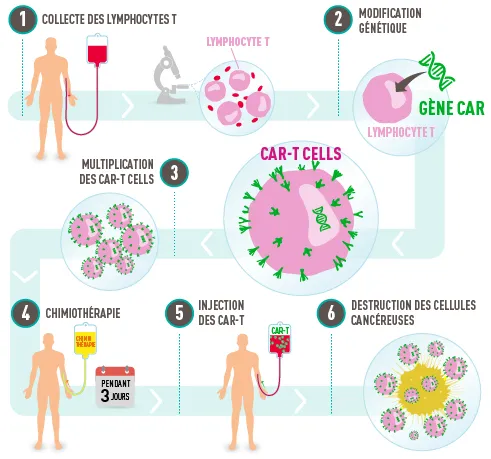
How CAR-T Cells work
- Collection: The patient’s T lymphocytes are collected through leukapheresis.
- Genetic Engineering: The T cells are modified ex vivo to express chimeric antigen receptors (CARs) along with a costimulatory molecule, enabling them to recognize tumor antigens and activate against malignant cells.
- Expansion: The modified CAR-T cells are expanded in culture
- Conditioning chemotherapy: regimen that promotes CAR-T cells proliferation and reduces the risk of rejection.
- Reinjection: CAR-T cells are reinfused into the patient
- Therapeutic Action: Once in the body, CAR-T cells specifically recognize and eliminate tumor cells expressing the targeted antigen.
Clinical Applications and Outcomes
CAR-T cell therapy offers a major therapeutic option for patients with acute lymphoblastic leukemia (ALL), diffuse large B-cell lymphoma (DLBCL), follicular lymphoma (FL) and multiple myeloma (MM).
Clinical studies report a complete response rate of approximately 40% in patients with refractory DLBCL, with sustained remission beyond two years in many cases.
Research and Future Perspectives
Since 2019, Gustave Roussy has been authorized to treat patients with CAR-T cells, with several individuals already benefiting from this therapy.
In parallel, clinical trials are exploring other forms of adoptive cell therapies, including TCR-engineered lymphocytes and tumor-infiltrating lymphocytes (TILs) to address solid tumors.
A New Therapeutic Horizon
CAR-T cells are opening new and promising avenues in oncology, providing hope for patients with treatment-resistant or relapsed cancers, and illustrating the power of precision immunotherapy developed at Gustave Roussy.
The CAR-T Cell Care Pathway